If you have been diagnosed with sleep apnea, your doctor will prescribe one of three main therapy types: APAP, CPAP, or BiPAP. They all work on the same principle of positive airway pressure, but the way each one delivers that pressure is different, and those differences matter for comfort, cost, and which patients each one suits best.
This guide compares APAP vs CPAP vs BiPAP head-to-head, explains the terminology, and walks through which therapy types are most commonly prescribed in Canada. We will also touch on ASV, a more specialized form of bilevel therapy used for complex cases.
Common PAP Therapy Terms Defined
Before comparing the therapies, here are the three terms that come up in every conversation about positive airway pressure:
- PAP (Positive Airway Pressure) is the underlying principle behind all three therapy types. A machine delivers air at a controlled pressure through a mask, which keeps the upper airway open and prevents the collapses that cause sleep apnea events.
- IPAP (Inspiratory Positive Airway Pressure) is the amount of pressure delivered when you breathe in.
- EPAP (Expiratory Positive Airway Pressure) is the amount of pressure delivered when you breathe out.
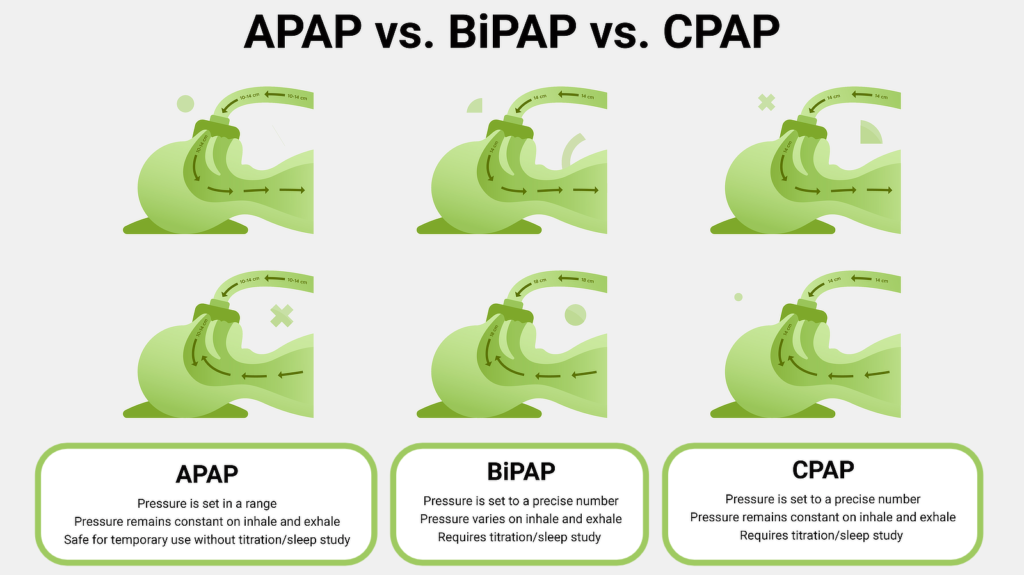
The differences between APAP, CPAP, and BiPAP come down to whether IPAP and EPAP are the same or different, and whether the pressure stays fixed or adjusts throughout the night.
APAP vs CPAP vs BiPAP: How Each Therapy Works
CPAP (Continuous Positive Airway Pressure)

CPAP machines deliver a single fixed pressure all night, with IPAP and EPAP set to the same value. The pressure level is determined during a sleep study or titration, and it does not change once you fall asleep.
CPAP pros:
- A simple, fixed-pressure therapy that has been the standard for decades
- The most straightforward PAP therapy to understand and operate
- Effective and well-tolerated for the majority of obstructive sleep apnea cases
CPAP cons:
- Requires a sleep study and titration to dial in the right pressure
- Some users find the constant pressure uncomfortable, especially when exhaling.
- Does not adjust if your needs change between sleep positions or sleep stages
In recent years, dedicated fixed-pressure CPAP machines have largely been phased out in Canada. Most modern APAP machines can be programmed to deliver a single fixed pressure, which means they can function as a CPAP when prescribed that way. As a result, what is dispensed today is almost always an APAP, even when the prescribed therapy is technically CPAP.
APAP (Auto-Adjusting Positive Airway Pressure)

APAP machines (sometimes called auto-CPAP) deliver pressure within a range your doctor prescribes, with the machine automatically adjusting up or down based on what your airway needs in real time. If you roll onto your back, enter REM sleep, or experience more events for any reason, the machine increases pressure. When the events ease up, it lowers the pressure for comfort.
Like CPAP, IPAP, and EPAP remain equal to each other at any given moment. The difference is that the value moves throughout the night.
APAP pros:
- Adjusts automatically for changes in sleep position, sleep stage, and night-to-night variability
- According to Lung Saskatchewan, an APAP automatically adjusts the pressure it delivers according to the person’s need, which makes it well-suited to people whose pressure requirements vary.
- The most commonly dispensed PAP machine in Canada, since modern APAPs can also operate as fixed-pressure CPAPs when prescribed
- Often more comfortable for people who find fixed CPAP pressures hard to tolerate
APAP cons:
- More expensive than a standard CPAP machine
- Highly dependent on a good mask seal, since the machine uses pressure data to decide when to adjust
- May not be the best fit for people with central sleep apnea or certain cardiac conditions
BiPAP (Bi-Level Positive Airway Pressure)

BiPAP machines (also called bilevel) take a different approach. Instead of one pressure for both inhale and exhale, BiPAP uses two: a higher IPAP when you breathe in, and a lower EPAP when you breathe out. Both values are set by your doctor and stay fixed throughout the night.
BiPAP is typically prescribed when CPAP or APAP have not worked well, when a patient needs higher pressures than they can comfortably exhale against, or when there are complicating conditions like COPD, congestive heart failure, or neuromuscular disease.
BiPAP pros:
- Easier to exhale against than CPAP or APAP, which improves comfort at higher pressures
- Helpful for patients with respiratory conditions or higher pressure requirements
- Can reduce aerophagia (swallowing air) that some users experience with continuous pressure
BiPAP cons:
- More expensive than CPAP or APAP machines
- Usually requires a more involved diagnostic and prescription process.
- Not necessary for most straightforward obstructive sleep apnea cases
ASV (Adaptive Servo-Ventilation)
ASV is a specialized type of bilevel therapy reserved for specific medical situations, primarily central sleep apnea, complex sleep apnea, and certain cardiac conditions. Like BiPAP, it uses different IPAP and EPAP pressures, but it also monitors your breathing pattern in real time and delivers additional pressure or even a backup breath if it detects a pause.
ASV is not a first-line therapy and should never be self-prescribed. It is also contraindicated for some heart failure patients, so the prescribing decision needs to come from a sleep specialist familiar with your full medical history.
Quick Comparison: APAP vs CPAP vs BiPAP
- Pressure delivery: CPAP is fixed and the same on inhale/exhale. APAP varies within a range, but inhale and exhale match. BiPAP keeps two separate pressures fixed for inhale and exhale.
- Best for: CPAP for typical obstructive sleep apnea. APAP for variable needs and travel. BiPAP for higher pressures, comfort issues, or complicating conditions.
- Cost: CPAP is the most affordable, APAP is mid-range, and BiPAP is the most expensive.
- Most common in Canada: APAP machines are the most commonly dispensed across Canada, since they can also be programmed to deliver a single fixed pressure when CPAP therapy is prescribed.
Which PAP therapy is best for me?
That depends entirely on your sleep study results, your medical history, and your personal comfort preferences. The Canadian Lung Association notes that your sleep specialist prescribes a particular pressure for you based on how much pressure you need to keep your airway open, and the right machine type follows from that prescription. Always consult your physician or sleep specialist before purchasing any PAP equipment.
Which PAP therapy is most commonly prescribed in Canada?
APAP machines are the most commonly dispensed PAP machines across Canada. Even when a doctor prescribes traditional CPAP therapy, the equipment supplied is usually a modern APAP set to deliver a single fixed pressure, since dedicated fixed-pressure CPAP machines have largely been phased out by manufacturers. The clinical decision between fixed-pressure and auto-adjusting therapy is still made by your sleep specialist, but the machine you take home will almost always be an APAP capable of either mode.
What are the most common side effects of PAP therapy?
Most side effects are minor and resolve as you adjust to therapy. Common ones include dry mouth or nose, nasal congestion, mask-related skin irritation, and aerophagia (swallowing air). Most are solved by adjusting humidification, swapping mask styles, or improving mask fit. Alberta Health Services notes that most people need a few weeks before they can sleep comfortably with their machine, and a few people have problems that take longer to sort out.
Do PAP machine settings need to be adjusted over time?
Once your pressure is dialed in through a sleep study or titration, the settings usually stay stable for years. Significant weight loss or weight gain, new medications, or new medical conditions can change your pressure needs, and in those cases, your sleep specialist may order a follow-up titration. Never adjust pressure settings yourself.
Do I need a prescription to buy a CPAP, APAP, or BiPAP machine in Canada?
Yes. All PAP machines are classified as medical devices in Canada and require a valid prescription from a licensed physician or sleep specialist. Masks, supplies, and accessories do not require a prescription.
Can I switch between CPAP, APAP, and BiPAP later?
Yes, but the switch should be made with your sleep specialist’s input. People often start on CPAP and move to APAP or BiPAP later if comfort issues arise, or if their medical situation changes. The new prescription will determine which machine type is appropriate.
Key Takeaways
- The differences between APAP vs CPAP vs BiPAP come down to whether the pressure is fixed or variable, and whether inhale and exhale pressures are the same or different.
- CPAP delivers one fixed pressure for both inhalation and exhalation. It is the simplest PAP therapy and remains the standard prescription for typical obstructive sleep apnea.
- APAP automatically adjusts pressure within a prescribed range. Modern APAP machines can also be programmed to operate as fixed-pressure CPAPs, which is why most patients in Canada are dispensed an APAP regardless of which therapy is prescribed.
- BiPAP uses two separate fixed pressures (higher for inhale, lower for exhale) and is typically prescribed when CPAP or APAP do not work well, or when complicating medical conditions are present.
- ASV is a specialized form of bilevel therapy reserved for central sleep apnea, complex sleep apnea, and specific cardiac conditions.
- The right therapy for you is determined by your sleep study, your prescription, and your sleep specialist’s clinical judgment. Never adjust your machine settings or change therapy types without medical guidance.
Need Help Choosing the Right PAP Therapy?
Whether you have just been prescribed CPAP, APAP, or BiPAP therapy, or you are considering an upgrade to a different machine type, our team is here to help. CPAPSupply.ca has been serving Canadians since 2013, and our staff includes a Registered Respiratory Therapist who can answer questions about machine types, prescription compatibility, and which models work best for different therapy needs. We will also work with your prescription to help you choose equipment that fits both your therapy and your budget.
